We’re leading a new approach in research, diagnosis, treatments and advocacy for PTSD and TBI.
By combining the power of biotechnology with rigorous research, high-performance computing, and data analytics, we’re accelerating the development of precision diagnostics and tailored treatments for military service members, Veterans, first responders, and all people living with the effects of brain trauma.
We advocate for people with brain trauma through a focused advocacy strategy that includes our Veterans Advisory Council, ongoing outreach to Congress, and dedicated educational programs.
Our goal is to advance tailored treatments for PTSD and TBI so that a clinician can target the right treatment to the right person at the time when they need help most.

Leveraging the right approach, the right tools, and the right partners.
CVB will achieve our mission to deliver solutions to people suffering from brain trauma by leading in multiple areas:

Research & Development
Researching and developing objective diagnostic tools that detect the underlying biology of brain trauma and treatments, including preventative wellness, digital health, drug and device approaches.
Collaboration
Convening the brightest minds in the PTSD and TBI research communities because collaboration, data sharing, and leveraging each partner’s unique capabilities is the fastest way to deliver impactful solutions to patients.


Tools & Platforms
Developing research tools & platforms which leverage our own technology and innovative approaches to enable our partners to conduct research that can scale & accelerate the development of effective solutions for brain trauma.
Advocacy
Shaping the environment for cutting-edge research by providing education to researchers on best practices and by fostering support for advancing brain trauma solutions at the federal, state and local levels through advocacy and education.

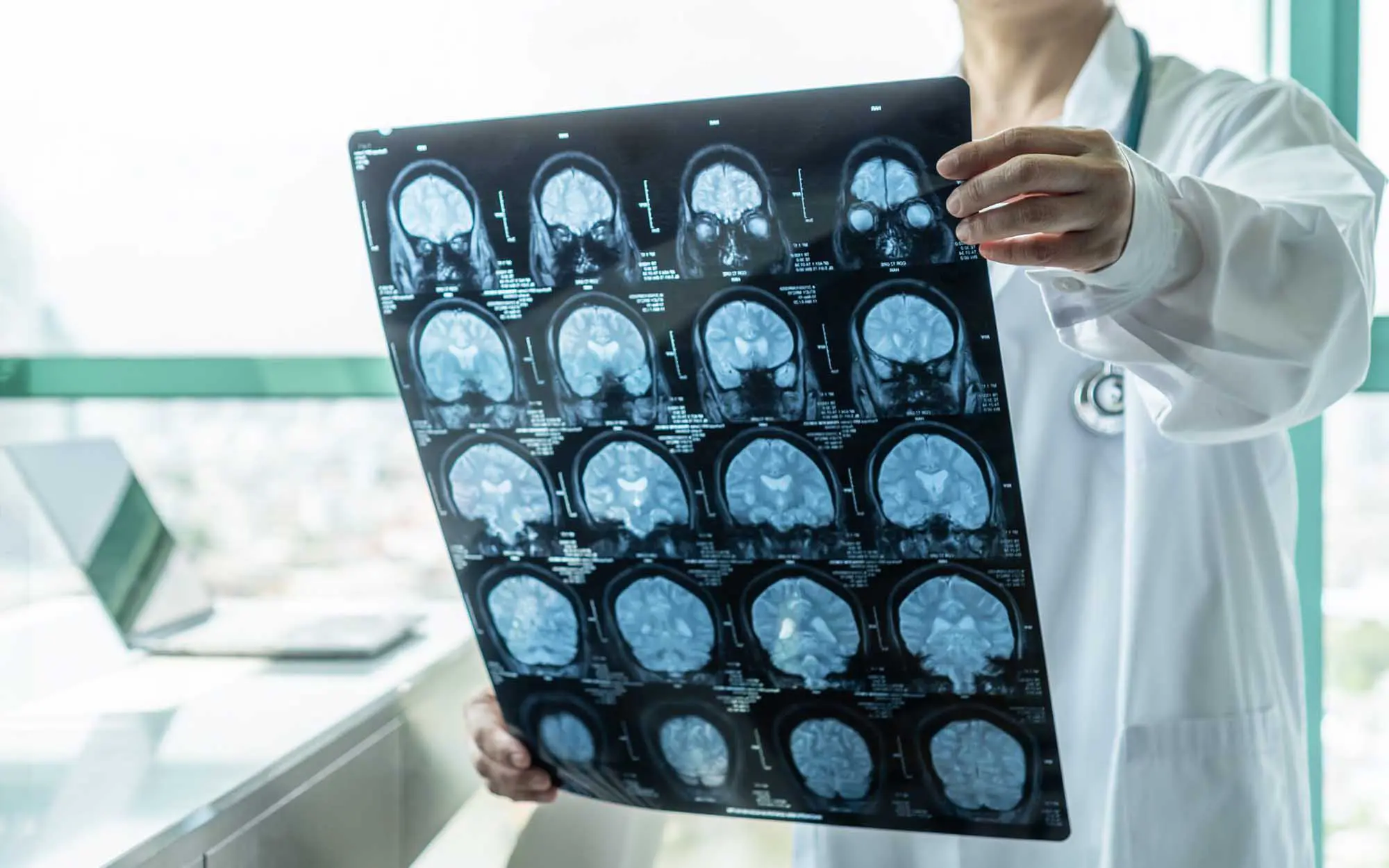
In the future we will be able to apply our discoveries to advance solutions to optimize brain health for all populations.
Learn more about our research here. Or make a difference and support our work by making a donation today.
Learn More About CVB

- About Us
Researchers & Partners

- About Us
Our Team

- About Us
News & Events

- About Us
Careers

- About Us
Veterans Advisory Council

- About Us















